Multimedia content
- Images (1)
- New ICUs set to open at hospitals across Lesotho
- All (1)
New ICUs Set to Open at Hospitals Across Lesotho
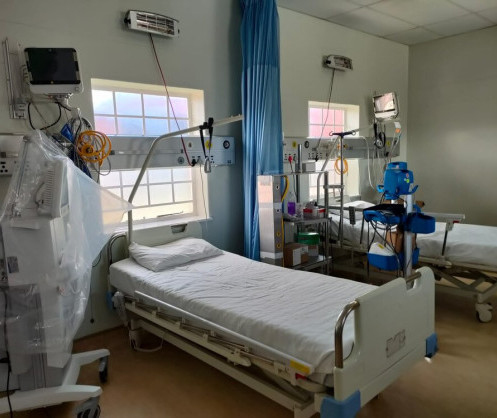
At Mafeteng Hospital in southwestern Lesotho, an eight-bed intensive care unit will feature a ventilator with piped oxygen and can accommodate a dedicated wing for COVID-19 patients
Hopefully after all the ICU needs have been met and there has been continued training for the staff, we will be able to care for critical patients
Critical care patients in Lesotho will soon be spared a trip to South Africa to receive treatment. The country is on the verge of opening its first intensive care units in public hospitals.
At Mafeteng Hospital in southwestern Lesotho, an eight-bed intensive care unit will feature a ventilator with piped oxygen and can accommodate a dedicated wing for COVID-19 patients. An oxygen plant is also on-site. The plant and oxygen supply is set to lower the cost of oxygen by up to 50%.
World Health Organization (WHO) has been training the doctors and nurses who will operate the new unit, which was funded by the World Bank. Five Ministry of Health staff, two doctors and three nurses, have been receiving training in admission criteria, oxygen therapy, high flow therapy, invasive mechanical ventilation, non-invasive mechanical ventilation, drugs management and COVID-19 critical and severe case management. They will become WHO-certified trainers themselves as the intensive care unit project expands.
“The trainings are theoretical and practical, using the material available in the hospital,” said Dr Raul Gonzalez Rodriguez, one of the trainers from the WHO Regional Office for Africa’s Case Management team.
Medical officer at Mafeteng Hospital, Dr Senate Mathaha, said the new unit would alleviate the care burden of trauma, diabetes, obstetric complications, HIV-related complications and now COVID-19.
“Taking care of ICU patients requires a lot of special skills on top of dedication and meticulous attention to detail,” she said, mentioning among them central line insertion, intubation, and operating machines like infusion pumps and ventilators.
“Hopefully after all the ICU needs have been met and there has been continued training for the staff, we will be able to care for critical patients,” she added.
At Berea Hospital in the north of the country, nurse and midwife Sello Ramakanate noted the improvements a new intensive care unit will bring for treatment of traumatic brain injuries, which are common in the area.
“Because of the mountainous terrain, and the use of donkeys and horses as modes of transport, the incidence of traumatic brain injuries is high. With limited access to health facilities, there is a relatively high occurrence of maternal and child related emergencies and some end up as deaths due to lack of critical care skills for the obstetric patients,” he said. “The use of alcohol and violence are also rife in Lesotho, particularly in areas where emergency care is limited and there is no capacity for intensive care. Life-threatening blood loss, head injuries and other conditions are prevalent, and some patients die because of the lack of a critical care unit.”
More ICU beds planned across Lesotho
Dr Francis Mupeta, a COVID-19 case management consultant for WHO in Lesotho, pointed out that there is a need for more ICU beds, as the country relied on South Africa for treatment in some cases.
“Critical patients would be evacuated to South Africa. I think the coming of COVID-19, and the lockdowns when South Africa was overwhelmed with critically-ill patients, exposed weaknesses in Lesotho’s healthcare. This ICU project is a step in the right direction in ensuring that critical care is paid attention to,” he said.
Dr Mupeta said the ICU project began when the government of Lesotho began to tackle the issues of increasing the capacity to treat critically-ill COVID-19 patients and reducing mortality due to COVID-19. A countrywide assessment, including the level of capacity for ICUs, identified only ten beds at private facility, which was prohibitively expensive for most of the population.
The project aims to increase intensive care unit beds to 36, located at various hospitals across the country, adding five to 10 beds per year.
Dr Pheello Ishmael Mobe, a General Practitioner at Berea Hospital and a trainee in this programme, said more skills development would be needed for the journey ahead.
“The more training we get, the better we will become at critical care. Through the experience of this training, when the ICU opens, we will be able to do mechanical ventilation. I hope with time our skills will get better to care for critical patients. Ultimately, Lesotho will benefit when the country is able to train more of its own specialists,” he said.
Dr Richard Banda, WHO Representative in Lesotho, said that COVID-19 has highlighted the gap in the treatment of the severe forms of the different diseases.
“ICUs are not only about COVID-19. ICU is about severity of the illness. All illnesses can develop into severe forms, and a universal health system should account for this. We will continue to work with our partners to close those gaps for a more equitable health system,” he said.
Distributed by APO Group on behalf of WHO Regional Office for Africa.